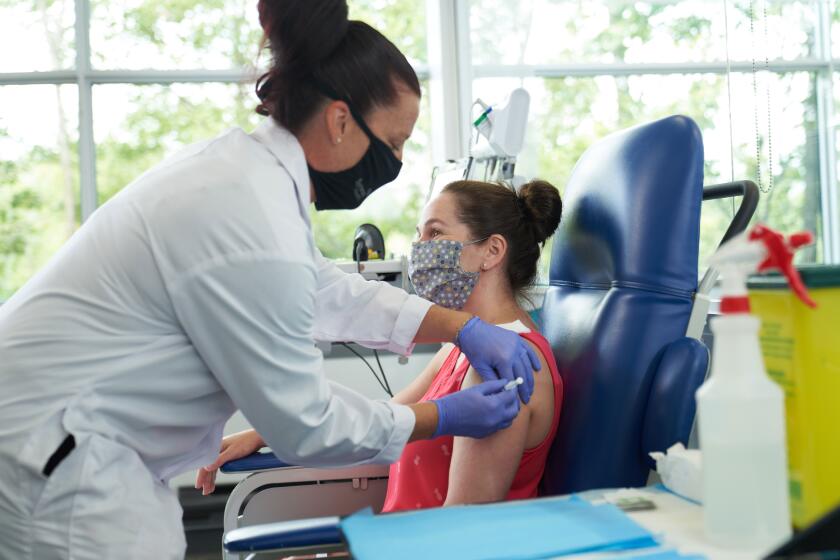
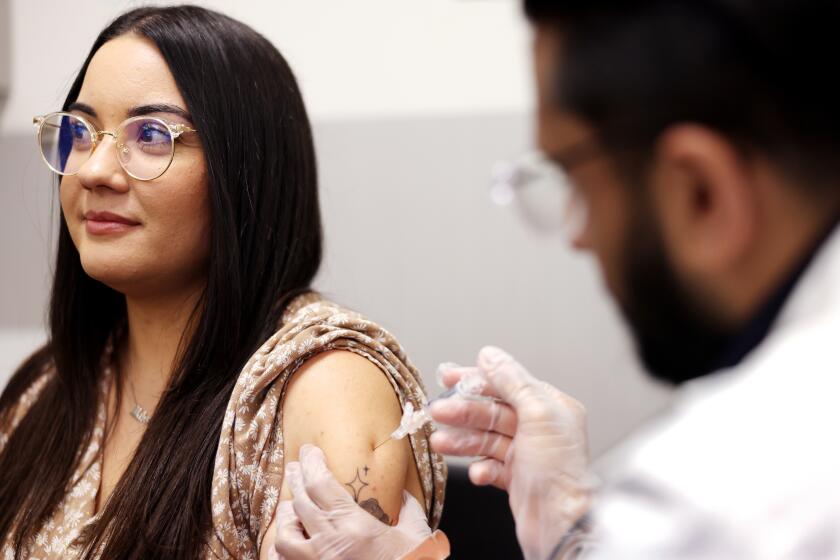
Health officials worry the U.S. isn’t ready for a COVID-19 vaccine

- Share via
Public health departments, which have struggled for months to test and trace everyone exposed to the novel coronavirus, are now being told to prepare to distribute COVID-19 vaccines as early as Nov. 1.
In a four-page memo sent last month, the Centers for Disease Control and Prevention told health departments across the country to draft vaccination plans by Oct. 1 “to coincide with the earliest possible release of COVID-19 vaccine.”
The CDC’s director, Dr. Robert Redfield, also wrote to governors last week about the urgent need to have vaccine distribution sites up and running by Nov. 1. Redfield asked governors to expedite the process for setting up these facilities, McClatchy first reported.
But health departments that have been underfunded for decades say they currently lack the staff, money and tools to educate people about COVID-19 vaccines and then to distribute, administer and track doses to some 330 million people. Nor do they know when — or if — they’ll get federal aid to help them do that.
“There is a tremendous amount of work to be done to be prepared for this vaccination program and it will not be complete by Nov. 1,” said Dr. Kelly Moore of the Immunization Action Coalition, a national vaccine education and advocacy organization based in St. Paul, Minn. “States will need more financial resources than they have now.”
Dozens of doctors, nurses and health officials expressed concern about the country’s readiness to conduct mass vaccinations, as well as frustration with months of inconsistent information from the federal government.
The gaps include figuring out how officials will keep track of who has gotten which doses and how they’ll keep the workers who give the shots safe.
With only about half of Americans telling pollsters they would get vaccinated, it also will be crucial to educate people about the benefits of vaccination, said Molly Howell, who manages the North Dakota Department of Health’s immunization program.
The unprecedented pace of vaccine development has left many Americans skeptical about the safety of COVID-19 immunizations. Others simply don’t trust the federal government.
“The message that is coming out is not a message of trust and confidence in medical or scientific evidence,” said Ann Lewis, CEO of CareSouth Carolina, a group of community health centers that serve mostly low-income people in South Carolina.
Food and Drug Administration and Centers for Disease Control and Prevention are under fire over decisions that seem based on politics, not science.
The U.S. has committed more than $10 billion to develop new coronavirus vaccines but hasn’t allocated money specifically for distributing and administering vaccines.
And while states, territories and 154 large cities and counties received billions in congressional emergency funding, that money can be used for a variety of purposes, including testing and overtime pay.
State and local public health departments across the U.S. have been starved for decades, leaving them underfunded and without adequate resources to confront the coronavirus pandemic. In addition, federal coronavirus funds have been slow to reach public health departments, forcing some communities to cancel non-coronavirus vaccine clinics and other essential services.
Many health departments are so overwhelmed with the current costs of the pandemic — such as testing and contact tracing — that they can’t reserve money for the vaccine work to come. Health departments will need to hire people to administer the vaccines and systems to track them, and pay for supplies such as protective medical masks, gowns and gloves, as well as warehouses and refrigerator space.
Arizona’s Pima County, for example, is already at least $30 million short of what it needs to fight the pandemic, let alone plan for vaccines, said Dr. Francisco Garcia, deputy county administrator and chief medical officer.
Some federal funds will expire soon. The $150 billion that states and local governments received from a fund in the CARES Act, for example, covers only expenses made through the end of the year, said Gretchen Musicant, health commissioner in Minneapolis. That’s a problem, given vaccine distribution may not have even begun.
Although public health officials say they need more money, Congress left Washington for its summer recess without passing a new pandemic relief bill that would include additional funding for vaccine distribution.
Then there’s the basic question of scale. For the U.S. to reach herd immunity against the coronavirus, most experts say the nation would likely need to vaccinate roughly 70% of Americans. That translates to 200 million people and — because the first vaccines will require two doses to be effective — 400 million shots.
“We’re not going to have 300 million doses all at once,” said Paul Mango, deputy chief of staff for policy at the U.S. Health and Human Services Department, despite earlier government pledges to have that many doses ready by the new year. “We believe we are maximizing our probability of success of having tens of millions of doses of vaccines by January 2021, which is our goal.”
Although the CDC has overseen immunization campaigns in the past, the Trump administration created a new program, Operation Warp Speed, to facilitate vaccine development and distribution. In August, the administration announced that McKesson Corp., which distributed H1N1 vaccines during that pandemic, will also distribute COVID-19 vaccines to doctors’ offices and clinics.
In preliminary guidance for state vaccine managers, the CDC said doses will be distributed free of charge from a central location.
The CDC spent two days working with vaccine planners in five locations — North Dakota, Florida, California, Minnesota and Philadelphia — to discuss potential obstacles and solutions. Those sessions have made Kris Ehresmann, who directs infectious disease control at the Minnesota Department of Health, feel more confident about who’s in charge of distributing vaccines.
“We are getting more specific guidance from CDC on planning now,” she said. “We feel better about the process, though there are still a lot of unknowns.”
The first wave of coronavirus vaccines might be like a flu shot, experts say, curbing symptoms in some patients but not protecting them from COVID-19.
When COVID-19 vaccines become available, health providers will need to track where and when patients receive their vaccines, because people will need to receive their second dose 21 or 28 days after the first, Moore said. And with many different shots in the works, they will need to know exactly which one each patient got, she said.
But many public health departments will struggle to adequately track who has been vaccinated and when because funding problems have left them in the technological dark ages, said Dr. Marcus Plescia, chief medical officer at the Assn. of State and Territorial Health Officials.
In Mississippi, for example, health officials still rely on faxes, said the state’s health officer, Dr. Thomas Dobbs. “You can’t manually handle 1,200 faxes a day and expect anything efficient to happen,” he said.
The CDC will require vaccinators to provide “dose-level accounting and reporting” for immunizations, so that the agency knows where every dose of COVID-19 vaccine is “at any point in time,” Moore said.
The CDC is developing an app for health departments whose data systems don’t meet standards for COVID-19 response, said Claire Hannan, executive director of the Assn. of Immunization Managers, a nonprofit based in Rockville, Md. “Those standards haven’t been released,” she said, “so health departments are waiting to invest in necessary IT enhancements.”
When vaccines are ready, health departments will need more staffers to identify people at high risk for COVID-19, who should get the vaccine first, Moore said. Public health staff also will be needed to educate the public about the importance of vaccines, as well as to administer shots, monitor patients and report serious side effects.
Plescia said people should be prepared for shortages, delays and mix-ups.
“It’s probably going to be even worse than the problems with testing and PPE,” he said.
Liz Szabo writes for Kaiser Health News (KHN), a nonprofit news service covering health issues. It is an editorially independent program of the Kaiser Family Foundation that is not affiliated with Kaiser Permanente. Associated Press writer Michelle R. Smith and KHN Midwest correspondent Lauren Weber contributed to this report.