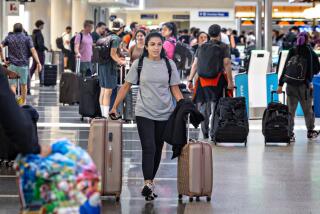COVID is rising in California. Here’s how to protect yourself from FLiRT subvariants

- Share via
There are growing signs of an uptick in COVID-19 in California thanks to the new FLiRT subvariants.
It’s far too early to know if FLiRT will be a major change in the COVID picture, and so far the impacts have been small.
But health officials are taking note and are urging Californians — especially those at risk — to be prepared.
In years past, summer travel and gatherings have spurred surges in coronavirus infections. As immunity wanes for those who received the most recent vaccine, experts urge caution.
Here’s rundown of what we know and how you can protect yourself.
What are FLiRT subvariants?
The FLiRT subvariants — officially known as KP.2, KP.3 and KP.1.1 — have overtaken the dominant winter variant, JN.1. For the two-week period that ended Saturday, they were estimated to account for a combined 50.4% of the nation’s coronavirus infections, up from 20% a month earlier.
Despite their increased transmissibility, the new mutations don’t appear to result in more severe disease. And the vaccine is expected to continue working well, given the new subvariants are only slightly different from the winter version.
“It’s been quite a while since we’ve had a new dominant variant in the U.S.,” Dr. David Bronstein, an infectious diseases specialist at Kaiser Permanente Southern California told The Times earlier this month. “With each of these variants that takes over from the one before it, we do see increased transmissibility — it’s easier to spread from person to person. So, that’s really the concern with FLiRT.”
What are officials seeing?
Doctors say they are not seeing a dramatic jump in severely ill people, and COVID levels still remain relatively low. But there are signs of a rise in infections that could lead to the summer coronavirus season beginning earlier than expected.
Over the seven-day period that ended May 20, about 3.8% of COVID-19 tests in California came back positive; in late April, that share was 1.9%. (Last summer’s peak test-positive rate was 12.8%, at the end of August.)
California may be headed to an earlier start to the summer COVID-19 season than normal as the latest family of coronavirus subvariants, FLiRT, has made significant gains nationally.
In San Francisco, infectious disease doctors are noticing more people in the hospital with COVID-caused pneumonia.
The Los Angeles County Department of Public Health has also started to see a very small uptick in cases in recent days. And Kaiser Permanente Southern California is reporting a small increase in outpatient COVID-19 cases.
How can I protect myself?
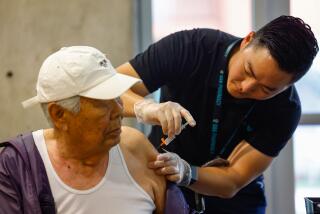
Vaccines
Doctors urged people to consider getting up to date on their vaccinations — particularly if they are at higher risk of severe complications from COVID-19.
In California, just 36% of seniors ages 65 and older have received the updated COVID-19 vaccine that first became available in September. The U.S. Centers for Disease Control and Prevention has urged everyone ages 6 months and older to get one dose of the updated vaccine. A second dose is also recommended for those ages 65 and older, as long as at least four months have passed since their last shot.
It’s especially important that older people get at least one updated dose. Of the patients he has seen recently who had serious COVID, said UC San Francisco infectious diseases specialist Dr. Peter Chin-Hong, all of them hadn’t gotten an updated vaccine since September, and were older or immunocompromised.
Behavior
Avoid sick people. Some sick people might pass off their symptoms as a “cold,” when it could be the start of a COVID-19 illness.
Testing
Test if you’re sick, and test daily. It’s sometimes taking longer after the onset of illness for a COVID-19 rapid test to show up as positive. Consider taking a rapid COVID test once a day for three to five consecutive days after the onset of cough-and-cold symptoms, said Dr. Elizabeth Hudson, regional chief of infectious disease at Kaiser Permanente Southern California. Doing so can help the sickened person take measures to later isolate themselves and limit spread of the illness to others.
Planning
Have a plan to ask for Paxlovid if you become ill. Paxlovid is an antiviral drug that, when taken by people at risk for severe COVID-19 who have mild-to-moderate illness, reduces the risk of hospitalization and death.
Masks are much less common these days but can still be a handy tool to prevent infection. Wearing a mask on a crowded flight where there are coughing people nearby can help reduce the risk of infection.
How can I protect my family and friends?
The U.S. Centers for Disease Control and Prevention has recently eased COVID isolation guidance, given that the health impacts of COVID-19 are lower than they once were, due to the availability of vaccines, anti-COVID medicines such as Paxlovid and increased population immunity.
There are fewer people getting hospitalized and dying, and fewer reports of complications such as multi-inflammatory syndrome in children.
Still, doctors say it remains prudent to take common sense steps to avoid illness and spreading the disease to others, given that COVID still causes significant health burdens that remain worse than the flu. Nationally, since the start of October, more than 43,000 people have died of COVID; by contrast, flu has resulted in an estimated 25,000 fatalities over the same time period.
While the prevalence of long COVID has been going down, long COVID can still be a risk any time someone gets COVID.
Here’s a guide on what to do if you get COVID-19:
Stay home and away from others while sick, plus a day after you’ve recovered
The CDC says people should stay home and away from others in their household until at least 24 hours after their respiratory viral symptoms are getting better overall, and they have not had a fever (and are not using fever-reducing medicine). Previously, the CDC suggested people with COVID isolate for at least five days, and take additional precautions for a few more days.
In terms of deciding when symptoms are getting better overall, what’s most important is “the overall sense of feeling better and the ability to resume activities,” the CDC says. A lingering cough by itself can last beyond when someone is contagious, the CDC said.
The Los Angeles County Department of Public Health also recommends testing yourself using a rapid test, and getting a negative result, before leaving isolation.
The agency also suggests staying away from the elderly and immunocompromised people for 10 days after you start to feel sick.
Take additional precautions after you recover in case you’re still contagious
People who have recovered from COVID-19 may still be contagious a few days after they have recovered. The CDC suggests taking added precautions for five days after they leave their household and resume spending time with others to keep others safe. They include:
- Wearing a well-fitting mask;
- Continuing to test for COVID-19. If positive, it’s likely you’re more likely to infect others, still;
- Keeping distance from other people;
- Increasing air circulation by opening windows, turning on air purifiers, gathering outdoors if meeting with people;
- And sticking with enhanced hygiene: washing and sanitizing hands often, cleaning high-touch surfaces, and covering coughs and sneezes.
Masking for 10 days to protect others
The L.A. County Department of Public Health says people with COVID-19 need to wear a well-fitting mask for 10 days after starting to feel sick, even if signs of illness are improving, to reduce the chance that other people could get infected. Masks can be removed sooner if you have two consecutive negative test results at least one day apart, the agency says.
Be aware of COVID rebound
COVID rebound can occur when people with COVID-19 feel better, but then start to feel sick two to eight days after they’ve recovered. Some people may also test positive again. COVID rebound can result in you becoming infectious again, capable of infecting those with whom you interact.
Rebound can happen whether or not you take Paxlovid.
Officials say if you feel sick again after having recovered from COVID, go back to following the same instructions to stay at home and away from other people during the first phase of the illness.
If you test positive but have no symptoms
The CDC says if you never had any symptoms, but test positive, take additional precautions for the next five days, such as masking up, testing, increasing air circulation, keeping distance and washing hands often.
The L.A. County Department of Public Health recommends wearing a well-fitting mask for 10 days after testing positive for COVID-19, and also avoiding contact with any high-risk people for 10 days after starting to feel sick, such as the elderly and immunocompromised people. You can remove your mask sooner if you have two consecutive negative tests at least one day apart.
If you are a close contact to someone with COVID-19
L.A. County health officials recommend close contacts of people who have COVID-19 wear a well-fitting mask around other people for 10 days after their last exposure. They suggest getting tested three to five days after their last exposure.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.